Tag: relationships
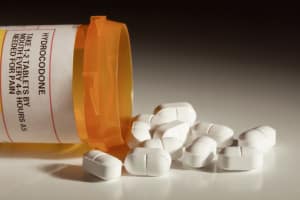
Opiates: A Painful Topic For Everyone
Todays Boston Globe has an article regarding physician prescribing of opiates to patients that have already experienced an overdose Opiate Prescribing to Patients With OD History. Between the documentary that HBO aired last night regarding the opiate crisis on Cape Cod and this article from today, I felt that as a primary care physician and as a resident of a seemingly “white-picket fence” suburb of Boston that has experienced its own opiate epidemic with the loss of too many good people- many of them kids-to this illness, it was worth commenting on. Many of these kids and young adults I knew and even played street hockey with as a kid. Others I did not know at all, but I can feel the loss when something like this happens.
I am not an Addiction Specialist or a Psychiatrist but as a Family Physician we do often deal with these issues and are usually the front door to the healthcare system. I have treated many patients that struggle with the disease of addiction and it is an extremely complex disease that is extremely difficult to cure and it usually coexists with other mental health diagnoses whether it be ADHD, major depression, anxiety disorders, bipolar disorder etc etc that add to the challenge. The hardest part of the disease to address initially is the denial. As a key cog in the wheels of this disease, denial is the toughest nut to crack. Just like any other chronic disease we treat, patients have to come to some degree of acceptance to move forward, and with addiction denial prevents this from happening easily. Sadly, we have no idea when that bridge of denial will be crossed and what the outlook on the other side looks like, but it needs to be crossed nonetheless.
I may be an idealist at heart and obviously have my biases, but I think one key solution to this epidemic is better primary care. People that struggle with the disease of addiction obviously need a multidisciplinary approach- one that includes doctors, nurses, social workers, counselors, addiction specialists etc- but they also need a primary care doctor that can help them navigate this messed up system, be the teams quarterback, and most importantly know them and treat them as a human being rather than just a “disease”. We need to ask the hard questions such as “with all the stories and news out there on this issue, what drove you to take that pill that started it all? what support system if any do you have? how can WE help YOU get healed? How do we as a community band together to educate and support our kids in a nonjudgmental supportive way? What are WE as a community doing wrong?” It isn’t all about the actual drug or the patient and the choices they have made. Its an US issue because it could be any of our friends, family members, or children that can succumb to this disease. And I don’t know about you but aren’t you tired of reading these obituaries week after week?
Our primary care system and mental health system need an overhaul for many reasons, but this epidemic is a big one. All patients of all socioeconomic backgrounds that struggle with this awful illness deserve better than 15 minute visits. They deserve better than more pills thrown at them. They deserve a relationship that is based on trust, care, and respect. What if the doctors that were studied in the aforementioned article had time to research records and databases during these visits? What if they actually had time to call other members of the patients care team? What if they had time to discuss the risks, benefits, and alternative options for pain management with their patients with appropriate, close followup and communication? I can personally attest to the fact working in the Direct Primary Care model has allowed me to treat patients with addiction 100% better. I have the time to listen, call other resources if needed, and followup frequently by phone or email. I am by no means perfect and do not always have success sadly. Yet there is one thing that DPC has allowed me to show the patient who struggles with addiction that all the Continuing Medical Education and seminars in the world do not even touch on and that is……that I too am an imperfect human being, that I do care, and that there is hope. I know this idealistic view will not solve the whole crisis, but maybe infusing some humanity towards these patients is a good start towards helping them heal and live a healthy life? What we are doing certainly is not enough and to me that is unacceptable.